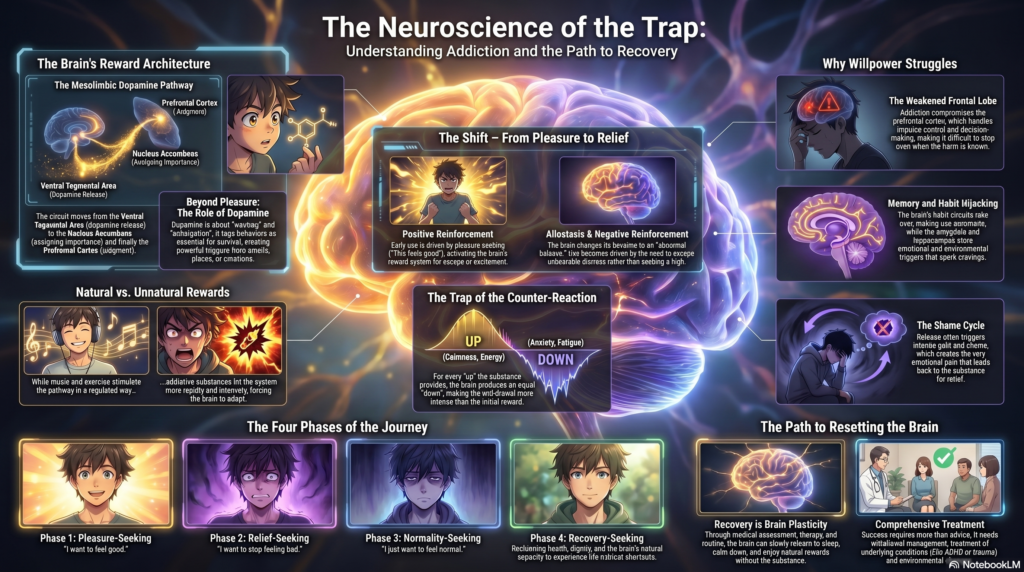
Why Addictions Are Hard to Give Up The Reward Pathway, Allostasis, and the Brain’s Search for Balance
 Addiction is not simply a problem of “weak willpower.” It is a disorder of reward, learning, stress, habit, memory, and self-control systems. The person may begin using a substance or behaviour for pleasure, relief, curiosity, peer influence, pain, sleep, anxiety, or performance. But with repeated use, the brain slowly changes its baseline.
Addiction is not simply a problem of “weak willpower.” It is a disorder of reward, learning, stress, habit, memory, and self-control systems. The person may begin using a substance or behaviour for pleasure, relief, curiosity, peer influence, pain, sleep, anxiety, or performance. But with repeated use, the brain slowly changes its baseline.
Over time, the person is no longer using only to feel good. They may be using to feel normal.
That is the key to understanding addiction.
The Brain’s Reward Pathway
The central reward pathway is called the mesolimbic dopamine pathway.
In simple terms:
Ventral Tegmental Area → Nucleus Accumbens → Prefrontal Cortex
The ventral tegmental area releases dopamine.
The nucleus accumbens gives the feeling of motivational importance: “This matters. Repeat this.”
The prefrontal cortex helps judge whether the action is good for long-term wellbeing.
Natural rewards such as food, sex, achievement, bonding, music, and exercise stimulate this pathway in a regulated way. Addictive substances and behaviours stimulate it more strongly, more rapidly, and often more unnaturally.
The brain then learns:
“This gives relief. This gives reward. Remember this. Repeat this.”
This learning becomes powerful.
Dopamine Is Not Just Pleasure
Dopamine is often described as the “pleasure chemical,” but that is incomplete.
Dopamine is more about:
- wanting
- seeking
- motivation
- anticipation
- salience
- reward prediction
- learning what to repeat
So addiction is not only about enjoying something. It is about the brain tagging that substance or behaviour as extremely important for survival-like relief.
This is why a smell, a place, a friend, a time of day, salary credit, loneliness, stress, or even boredom can trigger craving.
The brain remembers the pathway to relief.
From Pleasure to Relief
In the early phase, the person may use for pleasure.
They may think:
“This feels good.”
But after repeated use, the brain adapts. The same amount gives less pleasure. Natural rewards become less satisfying. Stress, restlessness, irritability, sleep problems, and emptiness increase when the substance is absent.
Now the person thinks:
“I need this to feel okay.”
This is the turning point.
Addiction shifts from positive reinforcement to negative reinforcement.
Positive reinforcement means:
“I use because it feels good.”
Negative reinforcement means:
“I use because not using feels unbearable.”
Long-term addiction is often driven more by relief from discomfort than by pleasure.
What Is Allostasis?
To understand why addiction becomes so persistent, we need to understand allostasis.
Homeostasis
Homeostasis means the body tries to maintain balance around a normal baseline.
For example, if body temperature rises, the body sweats to cool down.
The system returns to normal.
Allostasis
Allostasis means the body maintains functioning by changing the baseline itself.
In addiction, repeated substance use forces the brain to adjust. The reward system becomes less sensitive. The stress system becomes more active. The emotional baseline moves downward.
The person may now feel:
- low
- restless
- empty
- anxious
- irritable
- bored
- sleepless
- physically uncomfortable
without the substance.
So the drug or behaviour becomes part of the brain’s new abnormal balance.
This is why many patients say:
“Doctor, I am not taking it for enjoyment anymore. I am taking it just to function.”
That sentence captures allostasis beautifully.
The Brain Pushes Back
When a substance gives intense pleasure, calmness, confidence, stimulation, pain relief, or escape, the brain produces a counter-reaction.
If the substance gives euphoria, the later state may be dysphoria.
If it gives calmness, the later state may be anxiety.
If it gives energy, the later state may be fatigue.
If it gives sleep, the later state may be rebound insomnia.
If it gives pain relief, the later state may be increased pain sensitivity.
With repeated use, the positive effect becomes weaker, but the negative after-effect becomes stronger and longer lasting.
The person gets less reward but more withdrawal.
This is the trap.
The Three Stages of Addiction
A useful way to understand addiction is through three repeating stages.
1. Binge or Intoxication
This is the phase of use.
The reward system is activated. Dopamine and other neurotransmitter systems signal reward, relief, or excitement.
The person may experience:
- pleasure
- calmness
- confidence
- stimulation
- emotional escape
- social ease
- pain reduction
- temporary freedom from worry
The brain records the experience as useful.
2. Withdrawal and Negative Affect
After the substance wears off, the person feels worse than before.
This may include:
- craving
- anxiety
- irritability
- low mood
- insomnia
- body pain
- tremors
- sweating
- restlessness
- emptiness
- anger
- poor concentration
At this stage, the person is often not chasing pleasure. They are trying to escape distress.
The brain says:
“Use again. That is the fastest way to feel normal.”
3. Preoccupation and Anticipation
Before actual use happens, relapse often begins in the mind.
The person starts thinking:
“Only once.”
“I deserve it.”
“I can control it now.”
“I will stop from tomorrow.”
“Without it, I cannot sleep.”
“Without it, I cannot work.”
“This time will be different.”
This is not random thinking. It is craving, memory, stress, and habit working together.
Why It Is So Hard to Give Up Addictions
1. Natural Rewards Become Dull
After repeated overstimulation, the brain’s reward system becomes less sensitive.
The person may say:
“Nothing feels interesting.”
“Life feels boring without it.”
“I do not enjoy normal things anymore.”
“Even family, work, or hobbies do not give pleasure.”
This is not laziness. It is reward-system dysregulation.
2. Stress Becomes Harder to Tolerate
The addicted brain becomes more stress-sensitive.
Small problems feel bigger. Emotional pain feels unbearable. Sleep loss, criticism, loneliness, financial stress, relationship conflict, or work pressure can trigger craving.
The substance becomes the brain’s shortcut to relief.
3. Memory Keeps the Addiction Alive
The hippocampus remembers the context.
The amygdala remembers the emotion.
The striatum remembers the habit.
The prefrontal cortex struggles to control the impulse.
So the brain remembers:
- where to get it
- when to use it
- whom to use it with
- what emotion usually triggers it
- how quickly it gives relief
This is why old places, old friends, old routines, or old emotional states can trigger relapse even after months of abstinence.
4. Habit Circuits Take Over
In early addiction, the person may consciously choose the substance for pleasure.
In later addiction, the behaviour becomes automatic.
The person may say:
“Before I realized it, I had already bought it.”
“My body moved before my mind decided.”
“It has become part of my routine.”
This happens because addiction slowly shifts from reward circuits to habit circuits.
5. The Frontal Lobe Becomes Weaker at the Critical Moment
The frontal lobe is responsible for:
- judgment
- planning
- inhibition
- future thinking
- impulse control
- decision-making
- delaying gratification
In addiction, the frontal control system becomes weaker, especially during craving, stress, intoxication, or withdrawal.
This is why a person can know everything about the harm and still relapse.
The problem is not lack of knowledge.
The problem is that at the moment of craving, the reward-stress-habit system becomes stronger than the control system.
6. Withdrawal Teaches the Brain That Stopping Is Dangerous
Withdrawal is not just physical discomfort. It is a powerful learning experience.
The brain learns:
“When I stop, I suffer. When I use, I get relief.”
This makes the addiction self-reinforcing.
The person starts fearing abstinence itself.
7. Shame Worsens the Cycle
Many people relapse and then feel intense shame.
They think:
“I failed.”
“I have no control.”
“I am weak.”
“There is no point trying.”
This shame creates more emotional pain, and emotional pain becomes another trigger for use.
So the cycle becomes:
Use → guilt → shame → distress → craving → use again
Recovery requires breaking this shame cycle.
A lapse is not the end of recovery. It is information. It tells us where the vulnerable point is.
Substance-Specific Examples
Nicotine
Nicotine is strongly linked to daily cues: tea, coffee, driving, work breaks, phone calls, stress, and social situations.
Quitting becomes difficult because nicotine withdrawal causes irritability, poor concentration, restlessness, and craving.
The person feels:
“I cannot focus without it.”
Alcohol
Alcohol temporarily reduces anxiety, social discomfort, emotional pain, and insomnia. But repeated use worsens sleep quality, mood stability, impulse control, and anxiety over time.
The brain learns:
“Alcohol switches off distress.”
Eventually, alcohol becomes a relief-seeking behaviour rather than a pleasure-seeking behaviour.
Opioids
Opioids strongly relieve pain, emotional distress, and bodily discomfort. Withdrawal can be extremely uncomfortable.
The person may feel:
“Without it, my body and mind cannot tolerate life.”
This is why opioid dependence often needs medical treatment, not moral lecturing. Medicines such as buprenorphine-naloxone can stabilize receptors, reduce craving, and prevent the high-crash cycle.
Cannabis
Cannabis may initially feel relaxing or sleep-promoting. With repeated use, some people develop irritability, poor sleep, low motivation, anxiety, memory issues, or emotional dependence when they try to stop.
The person may feel:
“I need it to relax or sleep.”
Stimulants
Stimulants can create a powerful association with confidence, energy, productivity, sociability, or sexual performance. Withdrawal may cause fatigue, low mood, sleep disturbance, and loss of motivation.
The person may feel:
“Without it, I cannot perform.”
Behavioural Addictions
Gambling, gaming, pornography, social media, shopping, trading, and short-video scrolling can also affect reward systems.
They are powerful because of:
- novelty
- instant reward
- unpredictability
- variable reinforcement
- escape from boredom
- emotional numbing
- “just one more” loops
Variable reward is especially addictive because the brain keeps anticipating the next possible reward.
Why Willpower Alone Is Usually Not Enough
Willpower is important, but it is not enough by itself.
Addiction affects the very brain systems needed for willpower.
It weakens the frontal control system and strengthens reward, stress, habit, and cue-memory systems.
So recovery needs more than advice.
It needs:
- medical assessment
- withdrawal management
- craving control
- sleep correction
- treatment of depression, anxiety, ADHD, bipolar disorder, or trauma if present
- family support
- structured routine
- relapse prevention planning
- therapy
- environmental changes
- meaningful replacement rewards
The goal is not merely to stop the substance.
The goal is to help the brain rediscover natural balance.
Recovery Means Resetting the Brain
Recovery is the process of reversing allostasis.
The brain slowly relearns:
“I can sleep without it.”
“I can calm down without it.”
“I can enjoy life without it.”
“I can face stress without escaping.”
“I can feel normal again.”
This takes time.
But the brain is plastic. It can recover. Reward sensitivity can improve. Stress tolerance can improve. Frontal control can strengthen. Relationships can heal. Confidence can return.
A Simple Way to Explain Addiction
Addiction usually moves through three phases:
Phase 1: Pleasure-seeking
“I want to feel good.”
Phase 2: Relief-seeking
“I want to stop feeling bad.”
Phase 3: Normality-seeking
“I just want to feel normal.”
Treatment helps the person move into a fourth phase:
Phase 4: Recovery-seeking
“I want my life, health, dignity, and natural reward system back.”
Final Takeaway
Addiction is hard to give up because the brain changes its baseline. The reward system becomes less sensitive, the stress system becomes overactive, memory circuits preserve craving, habit circuits automate use, and the frontal lobe struggles to apply control at the crucial moment.
But these changes are not permanent destiny.
With the right treatment, support, structure, medication when needed, and compassionate relapse prevention, the brain can gradually reset.
Recovery is not just stopping a substance.
Recovery is rebuilding the brain’s capacity to experience life without needing an artificial shortcut to relief.
Need Help for Addiction or Substance Use?
Addiction is treatable. Whether the concern is alcohol, nicotine, cannabis, sleeping pills, opioids, prescription medications, gambling, gaming, pornography, or other compulsive behaviours, timely professional help can make recovery safer and more sustainable.
Dr. Srinivas Rajkumar T, MD (AIIMS), DNB, MBA (BITS Pilani)
Consultant Psychiatrist & Neurofeedback Specialist
Mind & Memory Clinic, Apollo Clinic Velachery (Opp. Phoenix Mall)
✉ srinivasaiims@gmail.com 📞 +91-8595155808
Related posts:
- Neurofeedback for Addiction: Retraining the Brain’s Reward Circuit Without Medication
- Allostasis and Addiction: Why It’s So Hard to Quit Alcohol and Other Substances
- OCD Direct and Indirect Pathway (CSTC) Circut
- The Dopamine Trap – Understanding Behavioral Addictions
- 🧭 Beyond Willpower: When to Seek Help for Behavioral Addictions
- BALANCE Study in Bipolar Disorder: Lithium vs. Valproate for Long-Term Maintenance